Cruel and unnecessary deaths
Last year 630 Australians died as a result of Hepatitis C. More will die, reports Graham Osborne, while the Pharmaceutical Benefits Advisory Committee rejects calls to make treatment affordable.
Australians are dying cruel and unnecessary deaths since a federal
advisory board rejected funding for breakthrough Hepatitis C (HCV)
treatment, say health experts.
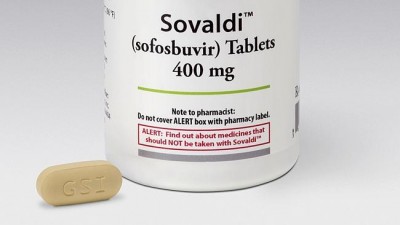
The new drug Sofosbuvir, marketed as Sovaldi, has shown an
unprecedented 90-95 percent success rate in curing HCV patients when
used in combination with other available drugs.
Pharmaceutical giant Gilead Sciences has priced its
“transformational” medicine at US$1,000 a pill or $US84,000 for a
12-week treatment. The company posted a record US$10.3 billion worth of sales of the drug in 2014 – its first year on the market.
The Therapeutic Goods Administration has approved Sofosbuvir for use
in Australia but the Pharmaceutical Benefits Advisory Committee (PBAC),
an independent body appointed by the Federal Government, last year
refused to subsidise the treatment, citing an “unacceptably … high
financial impact on the health budget.”
Gilead says in a statement that it’s now negotiating with the
committee and remains “optimistic” that the clinical benefits and
cost-effectiveness of Sofosbuvir will be recognised at the PBAC’s next
meeting.
The PBAC has refused to comment on the negotiations.
Australia is one of the few developed countries in the world that has
declined to subsidise Sofosbuvir for the most seriously ill HCV
patients.
“People are dying and others are getting sicker and sicker,” says Dr
Miriam Levy, the director of gastroenterology at Sydney’s Liverpool
Hospital.
“There’s a lot of people at the edge of the cliff and you really can’t predict which ones are going to fall off.
“It’s terribly cruel and completely unacceptable not to treat these
patients when there’s a drug that could cure them,” she says.
The Federal Government should follow the lead of the United Kingdom
and allow immediate access to the new treatment for urgent cases, says
Dr Levy.
“In the UK they’ve said, absolutely correctly, that
while they’re negotiating for a better price the people with cirrhosis
cannot afford to wait, so a special budgetary allocation was made to
allow treatment for clinically urgent cases.
“If someone would just give me 30 treatment courses now at Liverpool
Hospital. Let me deal with the sickest 30. Then we could meet again in
six months and think about broader access,” she says.
Many HCV patients don’t realise that they’re being denied potentially life-saving treatment, says Dr Levy.
“One of my patients is an army veteran who fought on the battlefields
for Australia. He has serious complications from cirrhosis and his
lungs are shutting down and he has no idea that he’s missing out on
something that could save his life. It’s just not right. This man fought
for his country.
“I didn’t train as a palliative care physician and that’s not my
brief, to support people in dying. But I’m being forced, as their liver
specialist, to provide best supportive care to people because we’re
living in a country where treatments are not available,” she says.
An estimated 233,000 Australians have chronic HCV infection,
according to the latest figures from medical researcher the Kirby
Institute. Of those, 80,000 have moderate to severe liver disease and
more than 600 people die every year.
“The only way we can stop this epidemic is to get broad access to
these new treatments for every Australian with the virus,” says Stuart
Loveday, CEO of health lobby Hepatitis NSW.
“It’s a shocking, life-threatening situation and, certainly, unnecessary deaths are happening.
“We are on the cusp of a treatment revolution and we could virtually
eliminate this blood-born virus from Australia within a generation but
we need the necessary tools right now to allow equal treatment access,”
he says.
It would be “much more cost-effective” to treat HCV in the short term
rather than to deal with significant increases in cirrhosis, liver
cancer, liver transplants and deaths that are expected in the next 15
years without the new treatments, says Loveday.
“Gilead did give 150 places for free for people on the liver
transplant list but many others have been left waiting and they’re
fearful that their liver disease will worsen and the delay could be
months or even years,” he says.
Patients are being driven to the brink and some are coping very badly, says Loveday.
“We’re hearing from an agitated and angry community of people who are growing increasingly desperate.
“They’re looking at their options and some are considering travelling
overseas to get the drugs at reduced prices or buying cheap drugs
online,” he says.
Dr Levy has warned patients about the dangers of online ads offering cheap Sofosbuvir treatments.
“The quality control could not be guaranteed and they could end up buying lolly water made in backdoor factories,” she says.
Australia’s health system is good enough that we should not be
forcing people into these kinds of desperate measures, says Loveday.
“We’re extremely disappointed that people living with Hep C in
Australia cannot access these new therapies and we think it’s unethical
to make them wait,” he says.
Loveday has called on the Federal Government and Gilead to
immediately resolve the impasse and says “the best chance for a leap
forward” will be at the PBAC meeting next month.
“The pharmaceutical industry is a little good/slash/evil and we just
need them to be a little less greedy,” says Gren, a 60-year-old mental
health researcher from Sydney who was first diagnosed with Hepatitis C
25 years ago.
Gren has undergone two treatments of the controversial HCV drug Interferon without success.
“The second Interferon treatment had so many spectacularly varied and
terrible side effects that it left me unable to work for 18 months and
now the virus that I can’t seem to shake is causing more and more
problems in my life.
“These new treatments are the most exciting thing that has happened
since I was diagnosed and they really are a revolution, a game-changer,”
he says.
But Gilead needs to go away and make a “cost adjustment,” says Gren.
“I recognise their right to make a profit and to return research
costs and all that but, I mean, how much profit? They’ve made record
profits out of this, billions and billions of dollars.
“Perhaps it’s time to reduce the price and alleviate people’s suffering.
“I do want the government to contain costs and I do want them to
negotiate on price but, on the other hand, these drugs are really good
and will cure a lot of people and we’re a wealthy country and we can
afford it,” he says.
Gren says he’s being forced to take early retirement because he’s
becoming too tired to turn up for work every day and too foggy to
concentrate on the work that needs to be done.
“I’m not angry…but talk to me again after the PBAC meeting next month
and I might be angry if they again refuse to subsidise this new
treatment. Obviously, there are no guarantees,” he says.
It’s important for HCV patients to stay positive while waiting for the treatment to become available, advises Dr Levy.
“The people who are infected must try to remember that this is the
beginning of a new dawn and it’s fantastic. This is a crazy situation
but we’ll get there.”
Graham Osborne is a freelance journalist who has written for The Sydney Morning Herald, SMH, AAP, 2GB, Media Monitors).
Interested in signing the petition to the Minister for Health to take urgent action to expedite the approval of new drugs for hepatitis C, including sofosbuvir?





No comments:
Post a Comment